How is the coronavirus (COVID-19) affecting prescription drug trends? Learn more.
Since March, when COVID-19 became an issue of national concern, we have seen a shift in how Navitus members are using their prescription benefits. Our clinical and analytics teams have been paying close attention to the data and the potential impact. Here are three trends they have observed.
#1 Increase in Overall Utilization
Within Navitus’ commercial line of business, we have seen an overall increase of 4% in prescription claims from January to July 2020. Maintenance medications are driving this increase while prescriptions for acute illnesses have actually declined.
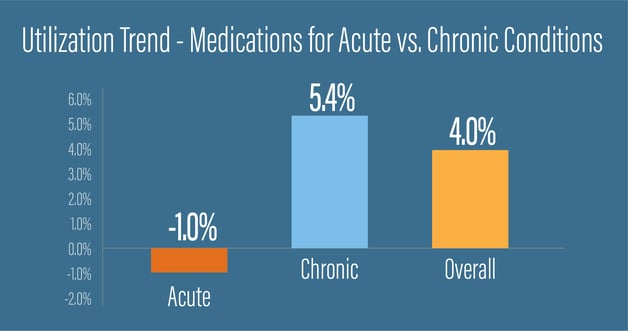
In general, this increase may have a positive effect on health outcomes as it appears that medical adherence for chronic conditions has improved.
#2 SHIFT FROM 30 TO 90-DAY FILLS
In March, we saw a 22% year over year spike in utilization. This increase was partially caused by relaxing Refill-to-Soon edits, which allowed members to fill their medication before refills were due. However, utilization dropped significantly in the following two months as Navitus provided pharmacies with a mechanism to determine whether an emergency fill was truly warranted. In turn, this is helping to reduce potential waste.
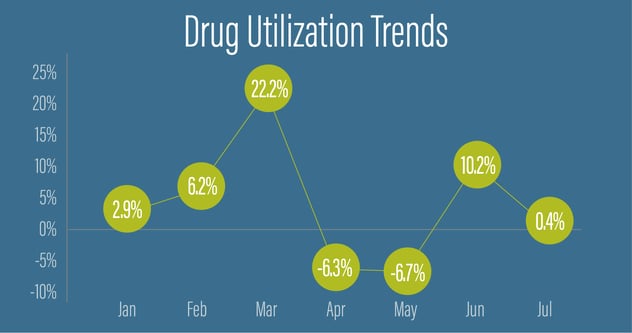
The other contributing factor was a shift in member purchasing behavior from 30 to 90-day fills. Following the initial spike, utilization subsequently dropped in April and May. By June, members who switched to a 90-day supply in March refilled their prescriptions again and we saw a corresponding increase of 10%.
Between January (pre-COVID-19) and June, we have seen an increase in the percentage of members participating in retail-extended or mail-order prescriptions. By the end of June, 28% of members are taking advantage of these services. We anticipate that the trend may continue as member behavior shifts to more convenient and cost-effective ways to manage their medications.
#3 Medications for Chronic Conditions Leading the Utilization Trend
In the past seven months, the increase in utilization has been driven by medications used to treat chronic conditions such as migraines, asthma, hypertension and diabetes. Below are the top categories for which utilization has increased, and the year over year increase:
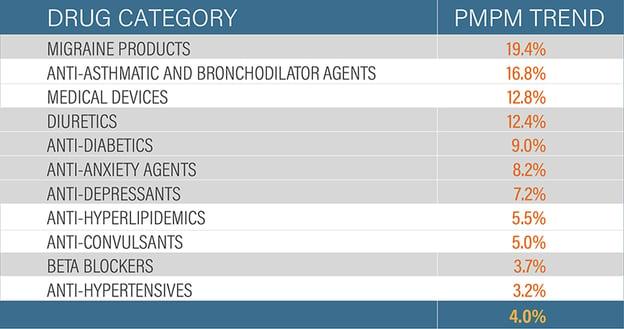
The drugs leading the utilization trend highlight two key points. First, they demonstrate members' willingness to comply with the protocols for chronic conditions. Second, the increase in migraine medications, anti-anxiety and anti-depressants also points to the mental strain the pandemic is having upon the population. Ultimately, maintaining optimal physical and mental health may help drive better health outcomes.
CONNECTING CLIENTS TO A BETTER SOLUTION
Prescription affordability continues to be a top issue in health care. With our business model of transparency with true pass-through pricing, an emphasis on the lowest net costs and improving health outcomes, we’re working hard to connect data and innovative ideas to develop meaningful solutions that meet the challenges of COVID-19 and beyond.
Want to learn how you can save 10-15% on your Rx benefits? Join us on September 23rd for a in-depth look at the latest trends in PBM contracts and the facts behind PBM transparency.

Source: Navitus Internal Data





